WASHINGTON, DC (May 7, 2020) –A novel workforce tool created by researchers at the George Washington University Milken Institute School of Public Health (Milken Institute SPH) estimates that the nation will need a total of 184,000 COVID-19 contact tracers in order to help society safely reopen and limit the size of future waves of the virus. The tool will help state and local health departments determine the number of staff needed to effectively identify and trace people who have been in contact with new cases of COVID-19 and slow the spread of the virus.
“We know the virus that causes COVID-19 is highly contagious and spread by human contact,” said Edward Salsberg, MPA, a senior research scientist at the Fitzhugh Mullan Institute for Health Workforce Equity (Mullan Institute), which is based at Milken Institute SPH. “This new tool will help public health officials plan for the workforce needed to identify those most at risk and ease up on community-wide social distancing measures yet still keep the public safe.”
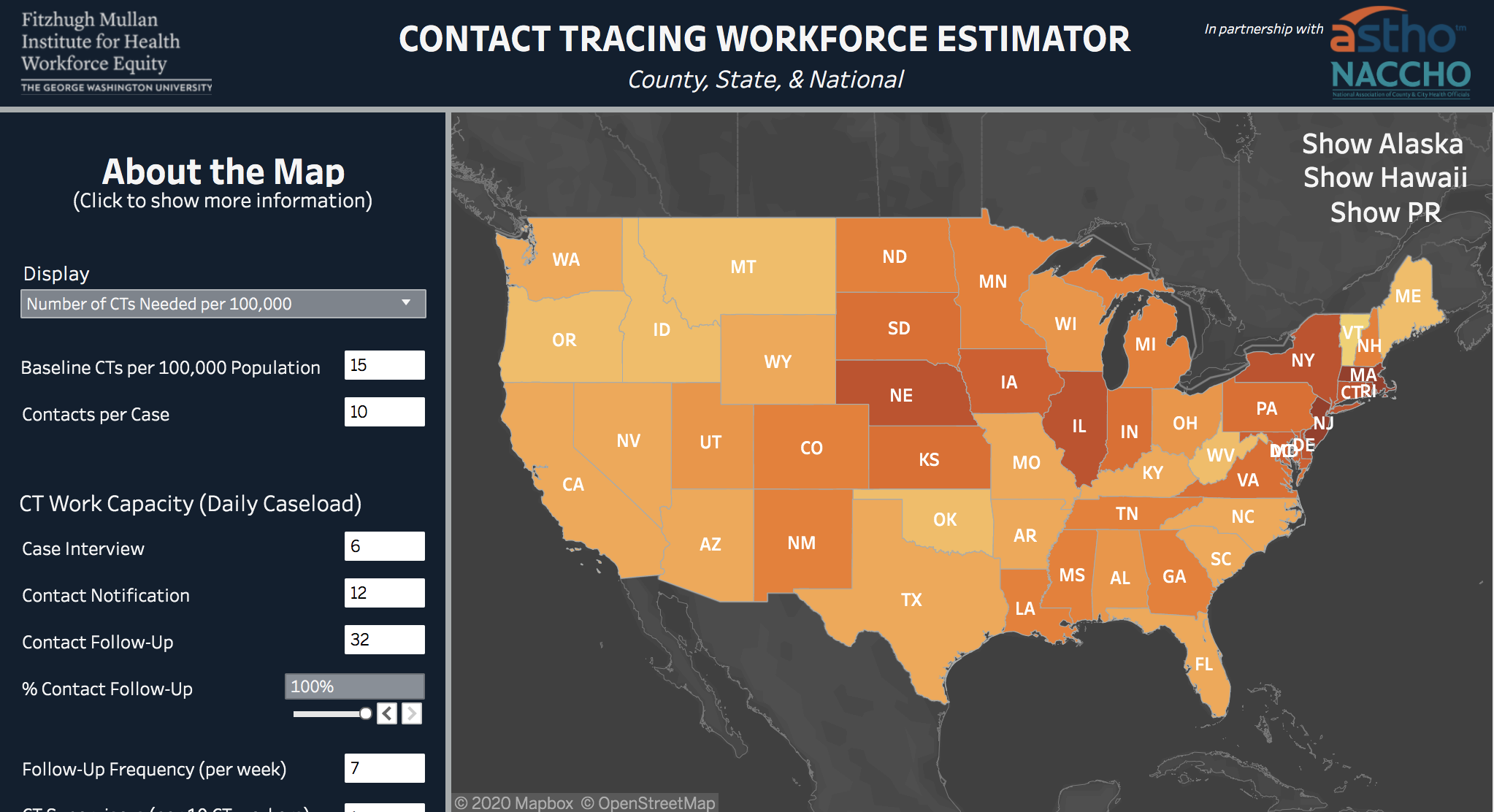
Using data on the number of COVID-19 cases, the estimated number of contacts per infected persons and other information, the team of researchers at the Mullan Institute have created the Contact Tracing Workforce Estimator. The tool was developed in collaboration with the Association of State and Territorial Health Officials (ASTHO) and the National Association of County and City Health Officials (NACCHO).
Using the new estimator, state and local public health officials will be able to plug in the number of COVID-19 cases and other data to help them gauge the number of staff needed to effectively trace contacts of all infected people in their jurisdiction. In addition, the estimator helps public health officials understand the factors, such as the need for social services, which can impact the number of contact tracers needed to slow the spread of infection.
Effectively stemming the viral spread requires that everyone in contact with a person who has tested positive is identified and contacted as soon as possible, ideally within 24 hours. A contact tracer provides information, recommends testing if that person has symptoms, and advises these individuals to quarantine for up to two weeks.
Up until now, lacking extensive testing and contact tracers, most communities in the United States have closed many businesses and schools and told students and employees to work or attend classes remotely. Public health experts know that social distancing and isolating people can help prevent the spread of the virus, but these blunt strategies also cause great economic and personal hardships.
To help pave the way for a safe reopening of restaurants, schools and businesses, state and local leaders need an expanded ability to test for the virus that causes COVID-19 and an army of contact tracers who can quickly identify people who have been exposed.
Recently, experts at ASTHO estimated that state and local health departments had only a few thousand contact tracers prior to the start of this pandemic—well below the number needed to confront the current cases of COVID-19. Without enough trained contact workers, infected people, including those who do not realize they have the virus, can spread the disease to many others in the community—a problem that could result in a second wave of infections.
“Returning to some semblance of normalcy is contingent on our nation’s public health capacity to contain future outbreaks through testing and contact tracing,” said Michael Fraser, chief executive officer at ASTHO. “Contact tracing is core work of state, territorial, local, and tribal public agencies. Public health does this type of work every day but there is an urgent need to scale up the workforce capacity needed to meet the challenge of COVID-19. This estimator tool will help health agencies prepare for the support they need in a more precise way using their local and state experience and capacity as a start.”
The contact tracing workforce includes case investigators, who interview people diagnosed with COVID-19 and then figure out how many people they might have come in contact with while contagious, and contact tracers, who notify and follow up with these contacts. Many workers have a public health background while others may complete focused trainings. Contact tracing has been used to quash emerging outbreaks of Ebola and SARS in the past and public health officials say that when coupled with adequate testing it could become a powerful method of preventing new cases of COVID-19—especially as the economy starts to reopen.
“Although state and local jurisdictions will soon begin to ease stay-at-home orders, this pandemic is far from over. As people are given the green light to patronize businesses and return to other public establishments, risk of COVID-19 transmission remains a threat,” noted Lori Tremmel Freeman, Chief Executive Officer at NACCHO. “As such, it is critically important for public health officials to be able to scale up and mobilize a well-trained contract tracing workforce with enough personnel to fulfill this important protective measure without overburdening or burning out the individuals doing the work.”
The Contact Tracing Workforce Estimator, was developed by a team at the Mullan Institute, including Candice Chen, Eric Luo, Nicholas Chong, Sara Westergaard, Clese Erikson, Patricia (Polly) Pittman and Edward Salsberg. The tool uses a unique combination of various factors to estimate the number of contact tracers needed to fight COVID-19.
This interactive tool and map project is supported by the Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services as part of an award totaling $450,000 with zero percentage financed with non-governmental sources. The contents are those of the author(s) and do not necessarily represent the official views of, nor an endorsement, by HRSA, HHS, or the U.S. Government. For more information, please visit HRSA.gov.